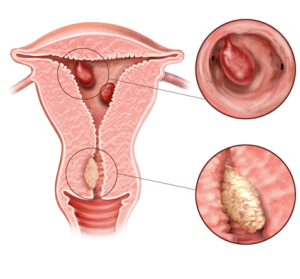
Endometrial polyps are tissue growths, usually benign, that arise from the endometrium lining in the uterine cavity. They can occur in a wide age range, from women of reproductive age to postmenopausal women. Most of the time they are asymptomatic, but in some cases they can cause problems such as abnormal uterine bleeding and infertility.
Endometrial polyps are abnormal tissue growths in the uterus, usually pedicled or broad-based (sessile), extending into the uterine cavity. They can vary in size from a few millimeters to several centimeters and can be either a single polyp or multiple polyps. Estrogen is thought to play an important role in the growth of these structures.
Although the exact causes of endometrial polyps are not known, some risk factors have been identified:
Although most endometrial polyps are asymptomatic, the following symptoms may occur.
Endometrial polyps are usually detected during routine gynecological examinations or infertility evaluations. Diagnostic methods are as follows:
Treatment is determined according to the size of the polyp, symptoms and age of the patient:
Monitoring rather than treatment is usually recommended in asymptomatic patients, small polyps and in the absence of significant risk factors in the pre-menopausal period.
Hysteroscopic Polypectomy: It is the gold standard in the treatment of endometrial polyps. The polyp can be removed together with its root, leaving no polyp tissue behind. It is a minimally invasive method and is usually performed under general anesthesia.
Dilation and Curettage (D&C): Although used to remove polyps, it is less effective than hysteroscopy and may not remove the entire polyp.
Hormone Therapy: Hormone therapy may be considered to regulate the balance of estrogen and progesterone.
Polyps after Tamoxifen Use: Due to the risk, regular follow-up is recommended and surgical intervention is performed if necessary.
Since the risk of malignancy (cancer) is higher in postmenopausal endometrial polyps, removal is generally recommended.
Endometrial polyps can create a mechanical barrier in the uterine cavity, making sperm passage or embryo implantation difficult. Surgical removal of polyps can improve the chance of pregnancy, especially in patients with a history of recurrent implantation failure or unexplained infertility.
Although endometrial polyps are usually benign, the risk of malignancy ranges from 0-3%.
Risk Factors: Large size of the polyp, occurrence in the postmenopausal period and presence of atypical cells increase the risk.
Recurrence: Polyps may recur in some patients. Regular follow-up is important.
Endometrial polyps are generally benign. However, the risk of cancer is around 0-3%, especially in polyps seen in the postmenopausal period, larger than 1.5 cm, bleeding or containing atypical cells. Therefore, a biopsy or polyp removal procedure should be performed in suspicious cases.
Some small and asymptomatic polyps may shrink and disappear over time, but most of the time they do not go away on their own. Medical or surgical treatment may be necessary, especially if there are menstrual irregularities, bleeding or infertility problems.
Hysteroscopic polyp removal is usually performed on a daily basis. Most patients return to their normal life within 1-2 days. There may be mild bleeding and cramping in the first few days. Complete recovery is usually achieved within 1 week.
Yes, polyps may recur in some patients. Especially if hormonal imbalance persists or if they are not completely removed, they may form again. Therefore, regular follow-up is recommended.
Depending on their location in the uterus, endometrial polyps can make sperm passage difficult or prevent the embryo from attaching. This can make pregnancy difficult. Removal of the polyp may increase the chance of pregnancy.
Polyps do not cause pain most of the time. However, pain may occur with very large polyps or with uterine contractions during menstruation. Abnormal bleeding is a more common symptom than pain.
If endometrial polyps are detected after menopause, they should be evaluated. Since estrogen production decreases during this period, polyps that develop should be monitored more carefully and removal is usually recommended.
If a symptomatic polyp or a polyp with a suspicious structure is not removed, bleeding problems may continue and there may be a rare risk of cancer. Therefore, the treatment plan recommended by the physician should not be neglected.
Yes you can. After the polyps are removed, the chance of pregnancy may increase, especially in women who have had infertility problems before. If there is no intrauterine adhesion after hysteroscopic polypectomy, the pregnancy plan can continue.
Untreated polyps:
Endometrial polyps are usually benign but can occasionally cause serious health problems. It is important for women with abnormal uterine bleeding, menstrual irregularities or pregnancy problems to consult a gynecologist without neglect. With early diagnosis and appropriate treatment, complications caused by polyps can be easily prevented.
If you would like to learn more about endometrial polyps or to determine the most appropriate diagnosis and treatment method for you, you can contact Prof. Dr. Şadıman Kıykaç Altınbaş, Obstetrician Gynecologist at her practice in Ankara. Being evaluated by an experienced specialist allows you to make the most accurate and reliable decisions about your health. You can contact us to make an appointment and get detailed information.

Kızılırmak, Dumlupınar Blv. No: 3 Next Level Ofis A Blok Kat: 14, No: 69, 06510 Çankaya/Ankara
Klinik: +90 538 430 32 10